Prescription Drug Benefits 2026: Navigating Part D Changes and Cost-Saving Strategies

Anúncios
Understanding the significant changes to Medicare Part D prescription drug benefits in 2026 is vital for seniors to navigate evolving costs and implement effective strategies for managing their healthcare expenses.
As we look towards 2026, the landscape of prescription drug benefits 2026 for seniors in the United States is poised for significant transformation. Medicare Part D, a crucial component of healthcare for millions of older Americans, will undergo pivotal changes designed to reduce out-of-pocket costs for beneficiaries. Navigating these updates effectively is paramount for seniors seeking to manage their medication expenses and ensure continued access to necessary treatments. This article will delve into the anticipated modifications, explore their implications, and provide actionable cost-saving strategies to empower seniors in this evolving environment.
Anúncios
understanding the medicare part d reforms for 2026
The year 2026 marks a critical juncture for Medicare Part D, with several major reforms set to take effect. These changes are primarily driven by legislative efforts to enhance affordability and predictability for beneficiaries, particularly those with high prescription drug costs. The aim is to alleviate the financial burden that many seniors currently face, ensuring that life-saving medications remain accessible without causing undue economic hardship.
One of the most impactful changes is the implementation of a $2,000 annual cap on out-of-pocket prescription drug costs for Medicare Part D enrollees. This cap represents a substantial shift from previous years, where there was no limit on how much beneficiaries might have to pay out of pocket once they entered the catastrophic phase. This new ceiling provides a crucial safety net, preventing seniors from facing exorbitant drug bills and offering greater financial security.
the $2,000 out-of-pocket cap explained
The introduction of the $2,000 out-of-pocket cap is arguably the most significant reform. Previously, after reaching the catastrophic phase of Part D, beneficiaries were still responsible for 5% of their prescription drug costs, which could amount to thousands of dollars for those with expensive medications. The new cap eliminates this 5% co-insurance, meaning that once a senior’s out-of-pocket spending on covered drugs reaches $2,000 in a calendar year, they will pay nothing for the remainder of that year.
Anúncios
- Reduced Financial Burden: This cap directly addresses the issue of high drug costs, providing a predictable maximum outlay for seniors.
- Enhanced Peace of Mind: Beneficiaries will no longer fear unlimited expenses for essential medications.
- Improved Adherence: Lower costs may lead to better medication adherence, improving health outcomes.
Furthermore, the structure of the catastrophic phase itself will see adjustments. With the elimination of the 5% co-insurance, the government and Part D plans will bear a greater share of the costs once the cap is met. This redistribution of financial responsibility is intended to make prescription drugs more affordable for those who need them most.
In essence, the 2026 reforms aim to create a more equitable and sustainable system for prescription drug coverage under Medicare Part D. By capping out-of-pocket expenses, the government is taking a proactive step to protect seniors from the escalating costs of necessary medications, fostering a greater sense of financial stability and access to care.
navigating the new part d benefit structure
The upcoming changes in 2026 will alter the traditional Medicare Part D benefit structure, requiring seniors to understand how their costs will be calculated and when they will reach the new out-of-pocket limit. This revised structure aims to simplify the system while providing more robust financial protection against high drug expenses.
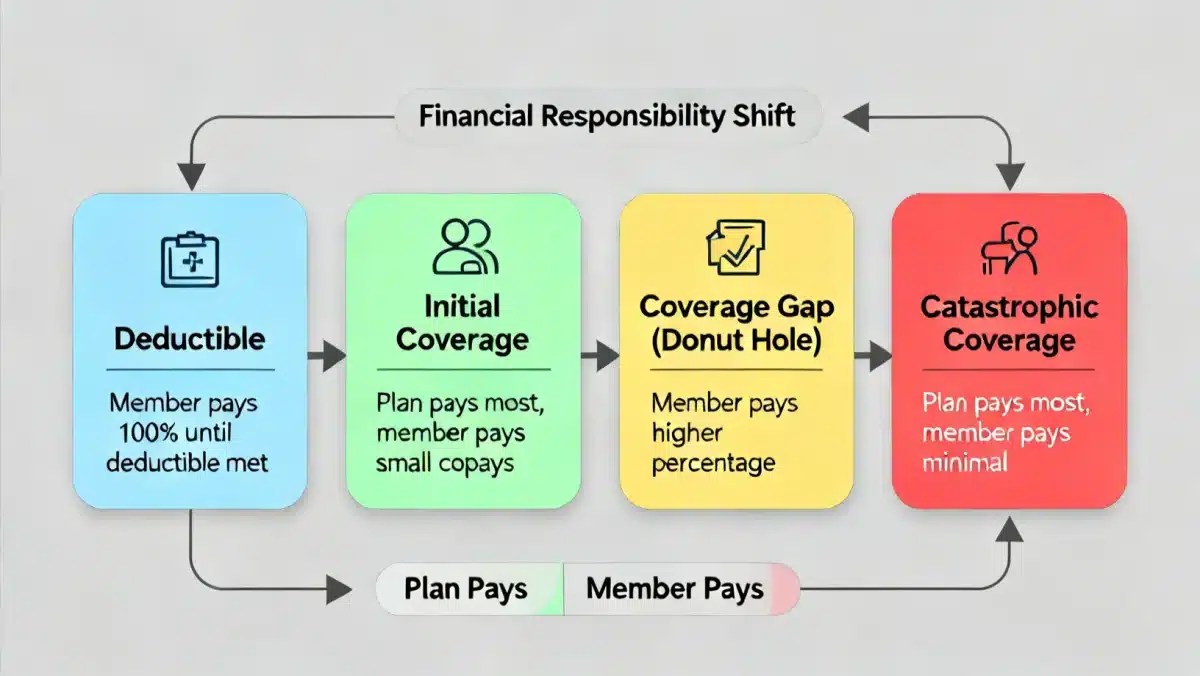
Currently, Part D has several phases: the deductible, initial coverage, the coverage gap (often called the ‘donut hole’), and catastrophic coverage. While these phases will largely remain, their financial implications for beneficiaries will shift significantly, particularly with the introduction of the $2,000 cap.
major shifts in coverage phases
The deductible phase is the initial amount you must pay out-of-pocket before your plan starts to pay. While the deductible amount may still vary by plan, the overall trajectory towards the out-of-pocket cap remains consistent. Once the deductible is met, you enter the initial coverage phase, where your plan pays a portion of your drug costs and you pay a co-payment or co-insurance.
- Initial Coverage Phase: You pay a co-pay/co-insurance; your plan covers the rest until a certain spending limit is met.
- Coverage Gap (Donut Hole): Once you and your plan have spent a combined amount (which changes annually), you enter the coverage gap. Here, you pay a higher percentage of the cost for most generic and brand-name drugs, though discounts are applied.
- Catastrophic Coverage: After your out-of-pocket spending (including what you paid in the deductible, initial coverage, and coverage gap) reaches a certain threshold, you enter catastrophic coverage. This is where the 2026 changes become most pronounced.
The critical difference in 2026 is that once your out-of-pocket spending reaches $2,000, you will move beyond the catastrophic phase and pay nothing further for covered prescription drugs for the rest of the year. This provides a clear ceiling on annual drug expenses, which was previously absent. It’s important to differentiate between total drug costs and your out-of-pocket spending; the $2,000 cap refers specifically to what you pay, not the total cost of the drugs.
Understanding these phases and how your spending accumulates towards the $2,000 cap is crucial for budgeting and planning. Seniors should carefully review their plan’s specific details, including deductibles and co-payments, to anticipate their potential costs throughout the year. The goal of these structural changes is to provide a more predictable and ultimately more affordable experience for beneficiaries.
strategies for minimizing prescription drug costs
Even with the new $2,000 out-of-pocket cap in place for 2026, seniors can employ several proactive strategies to further minimize their prescription drug costs. While the cap offers significant protection, being strategic about drug choices and plan selection can still lead to substantial savings throughout the year.
One of the most fundamental strategies is to regularly review your Medicare Part D plan. Plans can change their formularies (list of covered drugs), preferred pharmacies, and cost-sharing structures annually. What was the best plan for you one year might not be the most cost-effective the next. Open Enrollment, typically from October 15 to December 7 each year, is the prime time to make these evaluations and changes.
proactive plan selection and review
During Open Enrollment, utilize Medicare’s Plan Finder tool on Medicare.gov. This tool allows you to compare different Part D plans based on your specific medications and preferred pharmacies. It can help you identify a plan that covers all your drugs at the lowest possible cost, considering deductibles, premiums, and co-pays.
- Compare Formularies: Ensure your current medications are covered, ideally at a preferred tier.
- Check Pharmacy Networks: Verify if your preferred pharmacy is in the plan’s network, as out-of-network pharmacies can be more expensive.
- Calculate Estimated Annual Costs: The Plan Finder tool provides an estimate of your total annual drug costs for each plan, which is invaluable.
Another effective strategy involves discussing generic or lower-cost alternatives with your doctor. Generic drugs are chemically identical to their brand-name counterparts but are often significantly cheaper. If a generic option is available for your medication, asking your doctor if it’s a suitable alternative can lead to considerable savings. Similarly, some brand-name drugs have preferred status on plan formularies, meaning lower co-pays.
Furthermore, consider using mail-order pharmacies for maintenance medications. Many Part D plans offer lower costs or larger supplies (e.g., a 90-day supply for the price of two 30-day supplies) when using their preferred mail-order services. This can reduce both the per-pill cost and the frequency of refills, adding up to savings over time. By combining these proactive steps, seniors can significantly reduce their out-of-pocket expenses even before reaching the $2,000 cap.
impact on seniors with chronic conditions
The reforms to prescription drug benefits 2026 are particularly impactful for seniors living with chronic conditions. Individuals managing long-term illnesses often rely on multiple, sometimes expensive, medications daily. Historically, these individuals were disproportionately affected by the lack of an out-of-pocket maximum, frequently incurring substantial costs even in the catastrophic phase.
The new $2,000 annual out-of-pocket cap offers a profound sense of relief and financial predictability for this vulnerable population. No longer will they face the daunting prospect of unlimited drug expenses, which often forced difficult choices between medication adherence and other essential living costs.
enhanced financial security for high-cost users
For seniors with conditions like diabetes, heart disease, or certain autoimmune disorders, medication costs can quickly accumulate. Under the previous system, reaching the catastrophic phase meant still being responsible for 5% of drug costs, which could translate into thousands of dollars for highly specialized or branded drugs needed for chronic care. The elimination of this 5% co-insurance once the $2,000 cap is met provides a definitive ceiling on their annual spending.
- Predictable Budgeting: Seniors with chronic conditions can now budget for a maximum of $2,000 in annual drug costs.
- Improved Access to Care: Reduced financial barriers may allow for better access to necessary, often high-cost, specialty medications.
- Reduced Stress: Alleviates the significant financial stress associated with managing chronic illnesses and their associated drug regimens.
This change is expected to improve medication adherence among seniors with chronic conditions. When drug costs are a major barrier, some individuals may skip doses, split pills, or forgo refills, leading to poorer health outcomes. By capping costs, the reforms aim to remove a significant obstacle to consistent medication use, fostering better disease management and overall well-being.
Furthermore, the reforms may encourage more open discussions between patients and their healthcare providers about optimal treatment plans, knowing that the financial burden has a clear limit. This shift marks a significant step towards ensuring that seniors with chronic conditions can access the life-sustaining medications they need without facing insurmountable financial obstacles.
role of patient assistance programs and extra help
While the 2026 reforms to prescription drug benefits 2026 significantly improve affordability, patient assistance programs (PAPs) and Medicare’s Extra Help program will continue to play a vital role, especially for low-income seniors. These resources provide additional layers of support that can help reduce drug costs even further, potentially bringing them below the new $2,000 out-of-pocket cap.
The Extra Help program, also known as the Low-Income Subsidy (LIS), is a federal program that helps people with limited income and resources pay for their Medicare Part D premiums, deductibles, and co-insurance. For those who qualify, Extra Help can dramatically lower out-of-pocket costs, making essential medications much more affordable.
leveraging federal and pharmaceutical support
Seniors who meet specific income and resource guidelines should actively apply for Extra Help. Eligibility is often automatically granted to those who receive Medicaid, Supplemental Security Income (SSI), or help from their state to pay Medicare premiums. For others, an application can be submitted through the Social Security Administration.
- Reduced Premiums: Extra Help can cover part or all of your monthly Part D premiums.
- Lower Deductibles: It can also reduce or eliminate your Part D deductible.
- Minimal Co-pays: Beneficiaries typically pay very low co-pays for covered medications.
Beyond federal programs, pharmaceutical manufacturers often offer their own Patient Assistance Programs (PAPs). These programs provide free or low-cost medications to eligible patients who cannot afford their prescriptions. Eligibility criteria vary by program and are usually based on income, insurance status, and the specific medication needed.
Seniors should explore PAPs, especially for high-cost brand-name drugs that may not have generic alternatives. Your doctor’s office, social workers, or patient advocacy groups can often provide information and assistance with applying for these programs. Even with the 2026 cap, combining these assistance programs with the new Part D structure can lead to virtually no out-of-pocket costs for many eligible seniors, ensuring that financial constraints do not compromise necessary medical care.
preparing for the 2026 changes: a timeline for seniors
Effective preparation is key for seniors to seamlessly transition into the new landscape of prescription drug benefits 2026. While the changes are still a few years away, understanding the timeline and what actions to take beforehand can ensure you maximize your benefits and minimize any potential disruptions.
The most significant action period for seniors will remain the annual Medicare Open Enrollment, which occurs from October 15 to December 7 each year. During this time, you have the opportunity to review and change your Medicare Part D plan for the upcoming year. For the 2026 changes, this means paying close attention during the Open Enrollment period in late 2025.
key actions and dates to remember
Even before the 2025 Open Enrollment, there are steps you can take. Start by familiarizing yourself with the general outlines of the 2026 reforms. Resources from Medicare.gov, reputable senior advocacy groups, and trusted financial advisors can provide valuable insights. The more informed you are, the better equipped you’ll be to make strategic decisions.
- Ongoing Medication Review: Keep an updated list of all your prescriptions, including dosages and frequency.
- Financial Assessment: Understand your current income and resources, which is crucial if you might qualify for Extra Help.
- Consult Your Healthcare Providers: Discuss your medication needs and any potential changes with your doctors.
As 2025 approaches, pay close attention to official communications from Medicare and your current Part D plan. They will provide detailed information about how the 2026 changes will specifically impact your coverage and costs. During the 2025 Open Enrollment, utilize the Medicare Plan Finder tool extensively. Input your medications, compare plans, and pay close attention to the estimated annual costs under the new structure, especially how the $2,000 cap is factored in.
Consider seeking assistance from State Health Insurance Assistance Programs (SHIPs), which offer free, unbiased counseling on Medicare-related issues. These counselors can help you navigate the complexities of plan selection and ensure you choose the most suitable option for your unique health and financial situation under the new 2026 benefit structure. Proactive engagement with these resources will empower you to make informed decisions and optimize your prescription drug coverage.
future outlook and long-term implications
The 2026 reforms to prescription drug benefits 2026 represent more than just immediate cost savings; they signal a significant shift in the long-term approach to pharmaceutical affordability within Medicare Part D. These changes are part of broader legislative efforts to control healthcare costs and ensure sustainable access to medications for seniors for years to come.
One of the key long-term implications is the increased role of the federal government in negotiating drug prices. While direct negotiation for all drugs may be a gradual process, the initial steps taken suggest a move towards greater governmental leverage over pharmaceutical companies. This could lead to more competitive pricing and reduced overall costs for the Medicare program and beneficiaries.
evolving pharmaceutical landscape and policy
The $2,000 out-of-pocket cap could also influence pharmaceutical companies’ pricing strategies. With a hard limit on what beneficiaries pay, manufacturers might face pressure to adjust their pricing, especially for high-cost specialty drugs, as the financial burden shifts more towards insurers and the government. This could foster greater innovation in developing more affordable medications or drive companies to offer more robust patient assistance programs to maintain market share.
- Greater Price Transparency: Anticipate increased transparency in drug pricing as reforms take hold.
- Innovation in Affordability: Pharmaceutical companies may focus more on cost-effective drug development.
- Continued Policy Evolution: The 2026 changes are likely foundational, with further adjustments possible in subsequent years.
Furthermore, these reforms may encourage more seniors to enroll in Part D plans, knowing that their financial exposure is limited. This broader participation could lead to a larger risk pool, potentially stabilizing premiums and improving the overall financial health of the Part D program. The focus on affordability and access is expected to yield positive health outcomes, as fewer seniors will be forced to compromise on their medication needs due to cost.
In conclusion, the 2026 changes are a pivotal moment for Medicare Part D. They are designed to create a more equitable, predictable, and ultimately more affordable system for prescription drug coverage. While challenges and adjustments will undoubtedly arise, the long-term outlook points towards a more secure and accessible future for seniors’ medication needs, fostering better health and financial well-being across the United States.
| Key Aspect | Brief Description |
|---|---|
| $2,000 Out-of-Pocket Cap | New annual limit on what seniors pay for covered Part D drugs, eliminating 5% co-insurance in catastrophic phase. |
| Coverage Phase Adjustments | While phases remain, financial responsibilities shift, making catastrophic coverage more protective. |
| Cost-Saving Strategies | Regular plan review, generic alternatives, and mail-order pharmacies remain crucial for savings. |
| Extra Help & PAPs | Low-income subsidies and patient assistance programs offer additional support for eligible seniors. |
Frequently asked questions about 2026 part d changes
The most significant change is the implementation of a $2,000 annual cap on out-of-pocket prescription drug costs for beneficiaries. Once a senior’s out-of-pocket spending reaches this amount, they will pay nothing further for covered medications for the remainder of the year.
Seniors with chronic conditions, who often incur high drug costs, will benefit significantly from the cap. It provides financial predictability and protection, ensuring they won’t face unlimited expenses for their essential, often expensive, long-term medications.
Seniors should start preparing by staying informed now, but the critical period for action will be during the 2025 Medicare Open Enrollment (October 15 to December 7). This is when they can review and select a Part D plan that best suits their needs under the new structure.
Yes, patient assistance programs (PAPs) and Extra Help will remain vital. For low-income seniors, these programs can reduce costs even below the $2,000 cap, potentially leading to virtually no out-of-pocket expenses for their medications.
Utilize the Medicare Plan Finder tool on Medicare.gov during Open Enrollment. Compare plans based on your specific medications, preferred pharmacies, and estimated annual costs to find the most cost-effective option for your individual needs.
conclusion: a new era for senior prescription drug affordability
The impending changes to Medicare Part D in 2026 herald a new, more affordable era for seniors navigating prescription drug costs. The introduction of the $2,000 out-of-pocket cap is a monumental step towards providing crucial financial protection and predictability, particularly for those with chronic conditions or high medication expenses. While this reform significantly eases the burden, active engagement through informed plan selection, exploring generic alternatives, and leveraging available assistance programs will remain essential for maximizing savings. By understanding these pivotal shifts and proactively implementing smart strategies, seniors can confidently manage their healthcare expenses, ensuring continued access to the vital medications that support their health and well-being in the years to come.





